There’s no need to suffer incontinence in silence. FOF gets the scoop on new procedures that get rid of it for good.
In our mother’s generation, urinary incontinence was considered an unfortunate but inevitable part of getting older. A woman who experienced “leakage” kept her problem to herself and her bathroom cabinet stocked with Depends. Today, things are very different. If you’re one of the 20 million women who suffers from occasional, uncontrollable loss of urine, there are incredibly effective treatments that don’t involve the adult diaper aisle.
Unfortunately, this still isn’t a widely discussed topic (there’s no “walk for a cure” when it comes to incontinence) so many women don’t know how to get the best treatment. Fear not–we’ve done your homework for you. Last week, FOF met with Dr. Alan Garely, MD, one of the world’s leading experts on urinary incontinence and the Director of Urogynecology and Pelvic Reconstructive Surgery at Mount Sinai Hospital in New York. Dr. Garely answered every question–even the really embarrassing ones.
- What exactly is incontinence?
- There are two main kinds. Stress incontinence is defined as uncontrollable loss of urine when you exert yourself–cough, laugh or sneeze, for example. Urge incontinence is when you feel like you have a sudden urge to go, and you can’t hold it, so you leak.
- What causes it? Why is it more common for FOF women?
- Both women and men can become incontinent from neurological injury, birth defects, stroke, multiple sclerosis and physical problems associated with aging. As we age, the connective tissue in our bodies weakens and the muscles of the bladder and urethra start to stretch. Then we get leakage. Lack of estrogen may have a role in muscle weakness but that’s not definitive.
- Are some women at more risk than others?
- You are at higher risk if you…
- …had children vaginally. The more kids you have, the more risk you have, but one kid can do it.
- …have a chronic cough, like asthma or smokers cough.
- …have a genetic predisposition. if you have a family history of hernia, you have an increased chance of developing incontinence. Also, certain ethnicities are more prone, such as Irish, Northern European and Jewish.
- How do you treat it?
- Stress incontinence is almost always treatable with surgery, and there’s almost no non-surgical method that can treat it completely. You can do pelvic strengthening exercises, but that rarely cures the problem.
- Urge incontinence is usually treatable with medication, unless the vagina is prolapsing. Then, all the medication in the world won’t help you. A lot of people come into our office and say, “I have an overactive bladder problem but the medication isn’t helping…” and you examine them and you see the vagina is prolapsing.
- What is prolapse?
- It’s when the vagina begins to drop out of place. The best way to picture vaginal prolapse is to put your hand in your pocket and pull your pocket inside out–that’s prolapse. It’s similar to a hernia.
- How do you know if you have it?
- You need to have an exam, but most people notice a bulge coming out of the vagina. They feel pressure, or if they strain to have a bowel movement they feel like there’s something down there–a mass.
- Okay, so let’s assume I don’t have prolapse. I have stress incontinence and I leak when I laugh, cough, etc. What’s the treatment?
- As I said, surgery is pretty much the only way to fix it. There are a few approaches. The simplest would be injections–the doctor injects collagen around the opening of the urethra so that the urethra constricts and gets tight. That procedure is not very effective as a cure, and usually has to be repeated on a yearly or twice-yearly basis. The gold-standard of treatment for incontinence is called ‘a sling.’
- What’s that?
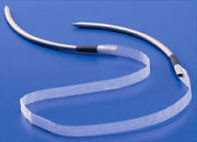
- A little piece of surgical mesh–made of a porous material called polypropylene–that’s inserted under the urethra so that it has support and you don’t have leakage. It’s placed under the skin–you don’t see it or feel it.
- You have to have surgery to put it in?
- Yes. The surgery is minimally invasive and takes about 10 to 15 minutes. The anesthesia is light–the same thing you’d get with a colonoscopy. There are two ways to do the surgery–one involves two tiny cuts right above the pubic bone and one in the vagina (called a TVT sling). The other involves two little cuts in the groin (called a TOT sling). The type you get just depends on your specific case. Both have a 90% cure rate.
- What’s the recovery time?
- Most people are continent immediately after the surgery. You can return to work within a few days…you just can’t lift a weight of more than 10 pounds for 8 weeks.
- How long has this surgery been available?
- It was first introduced in the United States in the late 1990s–it’s relatively new.
- I’ve heard there are risks to using mesh….is that true?
- The TVT and TOT sling surgeries I’ve described are very safe and effective. The FDA has issued a warning on all mesh procedures in the vagina. Unfortunately, they’ve lumped TVT and TOT together with a more risky surgery that’s used for vaginal prolapse. It involves a much bigger piece of mesh that can cause complications in about 15 percent of patients. What’s important to know is that TVT and TOT use only a small piece if mesh and their complication rates are very low.
- Okay, so what do I do if I have vaginal prolapse?
- We push the prolapse up, and the bladder leakage will clear itself up. That can be done with surgery or something called a pessary–a little ring that goes inside the vagina. Prolapse surgery involves a larger piece of mesh and can be done vaginally or abdominally. The complication rate for the prolapse surgery that’s done through the vagina–the risky one I mentioned before–is 45 in 300. The complication rate for the abdominal procedure is 1 in 300.
- Why would anybody opt for the prolapse procedure with the high complication rate?
- Because patients are under the belief that they want to avoid an abdominal incision at any cost. That’s not necessarily smart, but that’s their belief and sometimes it’s hard to convince people against their beliefs. Also, there are not many doctors who are trained to do the abdominal prolapse surgery–they may not even mention it as an option to their patients.
- You’ve said that the success of these incontinence surgeries has a lot to do with the skill of the surgeon. How do you choose a surgeon that you can trust?
- The one thing that has been proven to determine success rate more than anything else is the number of surgeries that doctor has done. The more surgeries, the better the outcome. Now, it’s hard to determine what someone’s numbers are unless they tell you, but you can always ask. It’s also important that your surgeon has done a three-year fellowship specifically in urogynecologic surgery.
- The American Urogynecological Society’s website, https://www.augs.org has a list of society members, and that’s a good place to start.
| Author | |
 |
Dr. Alan D. Garely, MD, FACOG, FACS, is the Director of Urogynecology and Pelvic Reconstructive Surgery at
The Mount Sinai School of Medicine in New York.
|


0 Responses to “Fix That Leak!”
Roxee910 says:
Has anyone had Da Vinci Robotic Surgery for Bladder Prolapse? I seem to be a candidate following a total hysterectomy in 1999. This newer type of surgery is done laprosopically with just 3 small incisions but it still requires a small amount of mesh.
I’m at the ‘should I’ or ‘shouldn’t I’ phase of my prolapse. Mechanically it’s a ‘should’ but emotionally I’m hesitant. Has anyone had this type of surgery?
baflour says:
I started with stress incontinence in the mid to late 90’s and had the sub-urethral sling done in 1999. The sling was made from tissue from my abdomen according to the surgeon. Around 2005, I progressed to urge incontinence. We have tried many different meds with no success. The idea of vaginal prolapse has never been mentioned, but, I will mention it at my next uro-gyne appt. Thanks for the insite.
sarahbaldwin says:
It’s a problem no one wants to talk about. Thank you for bringing the options into the light, and letting women know that we don’t have to suffer this embarrassing and inconvenient problem in silence. Thanks to Fab Over Fifty for this great article!
Charleigh says:
This is the most comprehensive and focused discussion of this topic I have ever seen — and, believe me, I’ve done some serious research! Thank you very, very much for providing this information. I’ve already passed this along to my cousin, and I know she will be grateful beyond measure.