Every year after having a mammogram at the Laura Perlmutter Center for Women’s Imaging at New York University Langone Health (that’s a mouthful!), I sit anxiously in the waiting room until I get the results. And, I breathe a sigh of relief when one of the employees informs me that the radiologist said everything looks “normal.”
That didn’t happen two weeks ago.
“The doctor wants another mammogram of your right breast,” said the young woman who pulled me aside with the news.
“What did they see?” I asked.
“I don’t have any details,” she responded, much like Siri would to a question on my iPhone.
Second mammogram taken, I return to the waiting room.
The bearer of news reappears and says, “I’m sorry, but we have to take the mammogram again. And we’re going to need an ultrasound. too. We’re waiting for your doctor to send in the prescription.”
Back for the third mammogram of the right breast, I think back to over a decade ago, when I two lumpectomies (one on each breast) after the radiologist saw something “suspicious.” Those procedures revealed benign calcifications in the breast. Will I be lucky a third time? I thought.
Two hours later, following the ultrasound, I am escorted to Dr. Heffernan’s office (she’s the radiologist), where the images of my breasts appear on the screen in front of her. She points out a cloudy area on the right image that wasn’t present on my 2016 mammogram, and explains that although it isn’t an actual tumor, the denser tissue could indicate malignant cells. Dr. Heffernan recommends that I next have an MRI, but emphasizes that what she’s seeing isn’t a major concern because it hasn’t spread. One cancer cell is serious, as far as I’m concerned, but I feel somewhat reassured. An MRI supposedly will provide a more definitive diagnosis.
It’s a Friday. The earliest I can have an MRI is the following week, since they need another prescription from my gynecologist before they can even make the appointment.
 I’m uneasy during the weekend, but correspond with my gynecologist, Dr. Mary Jane Minkin, from Yale New Haven Hospital and a professor at the Yale University School of Medicine, whose friendly warmth and intelligence put my mind at ease. I met Dr. Minkin about five years ago, when we both were working with a pharmaceutical company on a project concerning vaginal atrophy. I’d travel for hours to have her as my doctor.
I’m uneasy during the weekend, but correspond with my gynecologist, Dr. Mary Jane Minkin, from Yale New Haven Hospital and a professor at the Yale University School of Medicine, whose friendly warmth and intelligence put my mind at ease. I met Dr. Minkin about five years ago, when we both were working with a pharmaceutical company on a project concerning vaginal atrophy. I’d travel for hours to have her as my doctor.
First thing Monday, I’m fortunate to get an appointment for the MRI later that day. I can’t remember if I’ve ever had an MRI, but it’s no big deal. I’m positioned face down, massage style, and listen to the loud thumping of the machine for about 30 minutes while it goes to work.
Tuesday late morning, I get a call from someone at the office of Dr. Amber Guth, the breast surgeon who performed the two lumpectomies about 12 years ago.
“You have to have a biopsy,” the woman on the phone tells me matter-of-factly.
“Can I please speak to Dr. Guth,” I ask.
“No, you can’t talk to her until after she gets the biopsy report,” she admonishes me, in her best what-seems-like-20-something tone. “Besides, you’re a new patient.”
“Look,” I tell her as calmly as possible. “I am not a new patient, just because I’m no longer in your new electronic system. Dr. Guth performed two surgeries on me, and I want to know what’s going on.” By this time, I don’t know whether to laugh or cry.
Ms. Officious continues to deny me access to Dr. Guth, and refuses to read me the MRI report. I hang up. Talking to her, even for two minutes, is a complete waste of time, and it’s not going to help me to aggravate myself over her attitude.
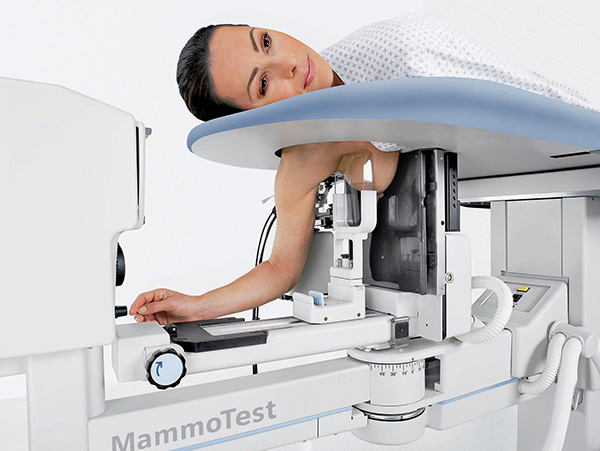
I then speak to an able, and clearly empathetic, assistant in Dr. Minkin’s office, who reads me the MRI report, which says that whatever they’re seeing is of “low suspicion” for malignancy. It recommends that I have something called a stereotactic biopsy, “a procedure that uses mammography to precisely identify and biopsy an abnormality within the breast. It’s normally done when the radiologist sees a suspicious abnormality on your mammogram that can’t be felt in a physical exam,” according to www.healthline.com.
![]()
Later in the day, I speak to Dr. Minkin, who assures me that “low suspicion” is good. “It takes cancer cells 10 years to grow into a tumor that you can see on a mammogram, and you don’t have a tumor,” Dr. Minkin explains. I figure time is on my side, based on the evidence. Even if the cells are malignant, they could be eradicated with treatment. Frankly, if they are cancerous, I want to have my entire breast removed. Why risk that one sneaky cell didn’t travel to another area of the breast and isn’t hiding out?
I also talk to my cousin, Dr. Joel Yellin, a breast surgeon in Rochester, NY, who tells me that most of these things turn out benign. Back to Google, I learn that I still have about a 10 to 13 percent chance that the cells are, indeed, cancerous. Not low enough for me, but neither would 1 percent be low enough.
I’m scheduled to have the biopsy tomorrow morning. I’ll let you know how it goes.
PS In the meantime, I receive a letter in the mail from the Laura Perlmutter Center for Women’s Imaging, which reads that my ultrasound was NORMAL. WTF, I think. I get nowhere when I call the center and try to get to get to the bottom of it. I’ll ask the radiologist about the letter tomorrow.


4 Responses to “My Perfect Timing For National Breast Cancer Awareness Month!”
karambir jangra says:
Health Line
Diet and wellness plus
nice post sir
İzmit Kurye says:
kurye izmit, https://www.izmitkurye.net
Rebecca Fornell says:
BEST OF LUCK GERI, Let’s stay positive. Early detection is the best prevention. Everything looks great so far.
GeriFOF says:
Thanks so much, Rebecca