This post is sponsored by Cyberonics, Inc.
Pamela, 62, spent a frightening decade with migraines, dangerously high blood pressure, forgetfulness, and tingling throughout her body.

During this time, her symptoms progressively worsened and included transient ischemic attacks (ministrokes) and weakness throughout her legs. Despite numerous lab tests, doctors in Atlanta couldn’t get to the root of Pamela’s problems and speculated that she had everything from multiple sclerosis to Lou Gehrig’s disease and Treacher Collins syndrome. They also prescribed medication after medication that proved ineffective. It wasn’t until Pamela took a sleep EEG, an exam that monitored electrical activity in the brain while she was asleep, that a neurologist was able to correctly diagnose her with epilepsy. Imaging of Pamela’s brain activity showed that, at times, she was experiencing as many as 80 seizures in a two-hour timeframe.
Epilepsy is a neurological disorder causing “sudden surges of electrical activity in the brain,” or seizures, according to the Epilepsy Foundation. Symptoms of seizures include loss of awareness (blacking out), confusion, loss of consciousness, tingling throughout the body, visual impairment, and many other bodily changes.
Epilepsy By The Numbers
Of the 3 million Americans with epilepsy, 300,000 are 60+, and more and more people are being diagnosed with the condition after they reach that age. According to the Epilepsy Foundation, at 75 years of age, three percent of the population will likely be diagnosed with epilepsy, and 10 percent of this same population will have had a seizure of some type. In contrast, only one percent will have developed epilepsy by age 20.

The after-effects of stroke, tumors or heart attacks are major causes of epilepsy, but epilepsy can occur in people of any age as the result of birth defects, injury or trauma to the brain, brain infections like meningitis, and even metabolic changes which restrict certain nutrients from reaching the brain.
How Is It Treated?
Four months after her firm diagnosis and even though she was taking six prescribed medications, Pamela’s symptoms were still occurring.
That’s when her doctor told her about something called VNS Therapy for drug-resistant (or refractory) epilepsy. Pamela was experiencing what one-third of people with epilepsy experience: drug-resistant epilepsy characterized by seizures that are not well-controlled with medication alone. While other options included brain surgery or a modified diet, Pamela and her doctor agreed that VNS Therapy would be the best treatment for her.
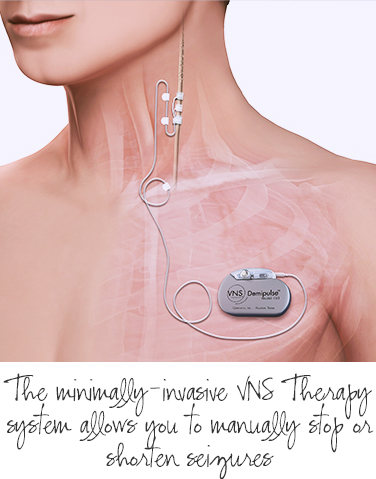
What Is VNS Therapy?
Vagus Nerve Stimulation (VNS) Therapy involves a minor procedure in which a small pacemaker-like device is placed under the skin in the chest and connected with a thin wire attached to the left vagus nerve in the neck. The vagus nerve is responsible for relaying messages between the brain and certain parts of the body, so this provides a minimally-invasive way to access the brain without brain surgery. The VNS Therapy system sends mild pulses through the vagus nerve indirectly to the brain to help regulate activity in the brain that can cause seizures. VNS Therapy also includes a hand-held magnet that can be placed over the small pacemaker-like device when the patient feels a seizure coming on (or during a seizure), to stop or shorten the seizure duration or intensity and to decrease the recovery time which occurs after the seizure stops. The therapy was approved by the FDA in 1997 and has been chosen by more than 80,000 people worldwide to help control their seizures.

With the addition of VNS Therapy, Pamela’s epilepsy is now under control, and she experiences seizures only rarely. She and her neurologist have been able to reduce her medication burden to only one now, and she is back to living an active life. “I’m a living example of the effectiveness of VNS. I volunteer, ride horses, and work every day.”
If you want to learn more about VNS Therapy, visit www.vnstherapy.com.
Background information for this article was provided by the Epilepsy Foundation and Cyberonics, Inc.

